

Published Apr 17, 2016
5 minute read
Dermal Filler Complications (Restylane/Juvederm)
There are several facial filler materials that have been approved by the Food and Drug Administration for use in the United States that have been employed by physicians for the past several years. These dermal fillers are very effective and popular cosmetic treatments for today's anti-aging and facial rejuvenation for aesthetic patients. One of the dermal fillers include hyaluronic acid, which is a ubiquitous carbohydrate polymer normally found as a major component of skin where it is involved in tissue repair. Hyaluronic acid injections temporarily smooth wrinkles by adding volume under the skin, with effects typically lasting for six months. Although they seem to be simple procedures, dermal filler complications may potentially occur.
Woman Getting a Botox Injection: Photo Courtesy of Ambro / FreeDigitalPhotos.net
These complications may include intraarterial embolization of hyaluronic acid (Juvederm & Restylane) which can have disastrous consequences. The dermal filler may be injected accidentally into tiny vessels if not performed properly by a trained medical professional. Intraarterial embolization of hyaluronic acid may lead to superficial to deep necrosis of the skin (premature death of cells and living tissues.) This will then lead to ulceration and severe deformity of the face. Embolization of dermal fillers may also lead to blindness, which is a rare complication.
How common is the facial necrosis complication from a dermal filler injection?
This complication is rare. The incidence of facial necrosis of the skin from a dermal filler injection (Zyderm/Zyplast collagen injection) was reported to be 9 in 10,000 cases. Facial skin necrosis may occur secondary to either intraarterial embolization or external compression of the small vessels of the skin by the dermal filler.
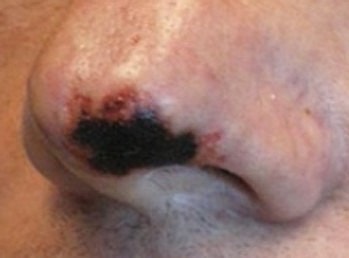 Necrosis of the tip of the nose from dermal filler injection into the nasolabial fold
Necrosis of the tip of the nose from dermal filler injection into the nasolabial fold
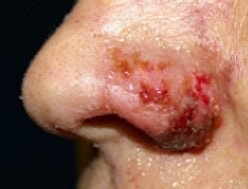 Complication from a dermal filler injection into the nasolabial fold
Complication from a dermal filler injection into the nasolabial fold
How can one treat intra-arterial injection of hyaluronic acid? Progression of the skin necrosis can be further prevented by injection of hyaluronidase (Amphadase) into the area of previous injection site. Thus, ask your provider if they have hyaluronidase in their office just in case a complication may arise.
How can one recognize this complication? One of the first few symptoms of intraarterial embolization of a dermal filler would be sharp pain and erythema (redness). The area of skin involved may vary from the local injection site to areas specifically supplied by the arterial vessel involved. This can be further recognized clinically by a bluish discoloration of the face that may eventually progress to necrosis and/or ulceration of the face.How can one avoid these potential dermal filler complications? It is very important for the medical provider performing these dermal filler injections to have a solid knowledge of the anatomy of the face to avoid injecting the dermal filler into the tiny vessels where embolization may occur. Moreover, the dermal filler should be injected into the correct plane and not deep enough to penetrate into the vessel. The level of injection is dependent on what one is trying to accomplish whether to improve a tear trough deformity or reduce perioral rhytids (wrinkle lines).
Once this complication occurs, can my provider fix the problem? Once necrosis/ulceration of the face occurs, injection of hyaluronidase into the previous injection site may prevent its progression. Once the necrosis has demarcated, your plastic surgeon may need to perform a plastic surgery procedure, such as debridement of dead tissue and possibly a reconstructive facial procedure. Whether you need a plastic surgery procedure or not is dependent on the severity and location of the ulceration/skin necrosis of the face.
Other Potential Complications of Dermal Fillers
I recommend that one should ask one of your Houston plastic surgeons for these potential complications from injectible dermal fillers, such as Restylane and Juvederm, prior to undergoing such procedures. One should also ask their plastic surgeon that if such complications arise, what can be done to minimize and correct the adverse outcome that can potentially happen. Being able to recognize, prevent and treat these potential complications are essential, even for a minor procedure such as a dermal filler injection.
I recommend reading about Botox for dynamic wrinkles.
Other Recommended articles:
"To create something exceptional, your mindset must be relentlessly focused on the smallest detail." ~ Georgio Armani
Reference:
The Aesthetic Meeting 2010 by the American Society for Aesthetic Plastic Surgery Bailey S., Cohen J., and Jeffrey Kenkel. Etiology, Prevention, and Treatment of Dermal Filler Complications. Aesthetic Surgery Journal January 14, 2011 vol. 31 no. 1110-121 Glaich, et al. Injection necrosis of the glabella: protocol for prevention and treatment after use of dermal fillers. Dermatol Surg. 2006 Feb;32(2):276-81.Grunebaum, et al. The risk of alar necrosis associated with dermal filler injection. Dermatol Surg. 2006 Feb;32(2):276-81.
Hanke, C. W., Higley, H. R., Jolivette, D. M. et al. Abscess formation and local necrosis after treatment with Zyderm or Zyplast collagen implant. J Am Acad Dermatol. 25: 319, 1991.
Inoue, et al. Arterial embolization and skin necrosis of the nasal ala following injection of dermal fillers. Plast Reconstr Surg. 2008 Mar;121(3):127e-128e.
Lemperle, et al. Avoiding and Treating Dermal Filler Complications. Plast Reconstr Surg. 2006 Sep;118(3 Suppl):92S-107S.
Other articles related to dermal fillers:
1) The Facts about BOTOX 2) Are You a Good Candidate for BOTOX? 3) Dermal Fillers (Juvederm | Restylane | Radiesse) 4) Which Dermal Filler is Best For Me?